The next NephJC Monday February 6 at 9 pm EST. We will be using #JHMChat
Cost of Acute Kidney Injury in Hospitalized Patients
Samuel A. Silver, MD, MSc, Jin Long, PhD, Yuanchao Zheng, MS, Glenn M. Chertow, MD, MPH
Background
Acute kidney injury (AKI) is common, deadly and expensive. We know how common it is, it occurs in roughly 20% of hospitlaized patients. We know how deadly it is, it has a mortality of 20-25% and if the patient is in the unit and requires dialysis the mortality will grow to over 50%. But though we know it is expensive we our data on just how expensive is a bit cloudy.
Chertow did a single center study on the cost of AKI in 2005 that found AKI was expensive but the number of patients with severe AKI was relatively modest (only 105 patients had an increase in creatinine of more than 2 mg/dL).
The main objectives of this study were to determine the costs of AKI-related hospitalization, and patient and hospital factors associated with these costs.
Methods
The data is from the National Inpatient Sample. This is a nationally representative administrative database of hospitalizations in the United States created by the Agency for Healthcare Research and Quality as part of the Healthcare Cost and Utilization Project. They looked at the 2012 NIS subset.
“The 2012 NIS subset contained administrative data from over 7 million hospitalizations, representing more than 4000 hospitals, 44 states, and 95% of the US population.”
They excluded ESRD patients and patients under the age of 18.
AKI was identified by ICD-9 codes, a method validated to be highly specific at the cost of decreased sensitivity. AKI with dialysis (AKI-D) was defined as having an AKI diagnosis and either a diagnosis or procedure code for dialysis. This method has been validated to be both sensitive and specific.
They calculated the mean increase in cost and length of stay (LOS) of each hospital record, comparing hospital records with AKI and AKI-D to hospital records without AKI. The primary outcome was the inpatient cost of each hospital record in 2012 dollars.
Results
The data base contained 36,484,846 patient records. After excluding ESRD they were down to This was reduced to 29,763,649 inpatients, of which 3,031,026 had AKI, 10.2%, of which 106,515 (3.5%) required dialysis, 0.36%.
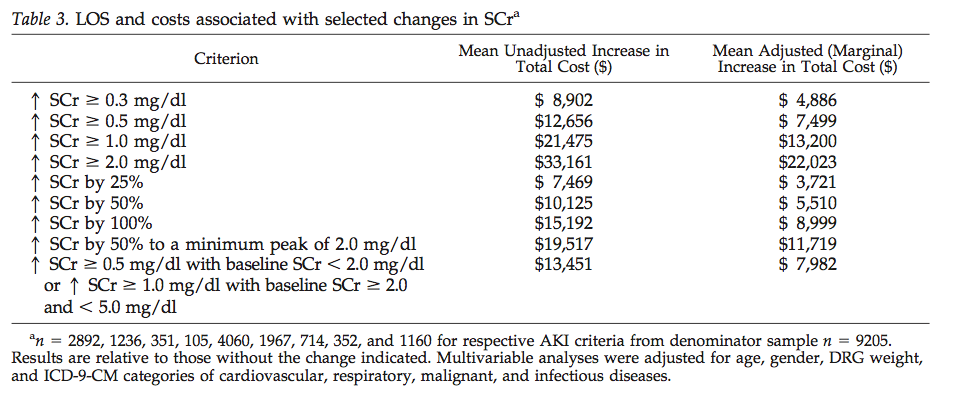
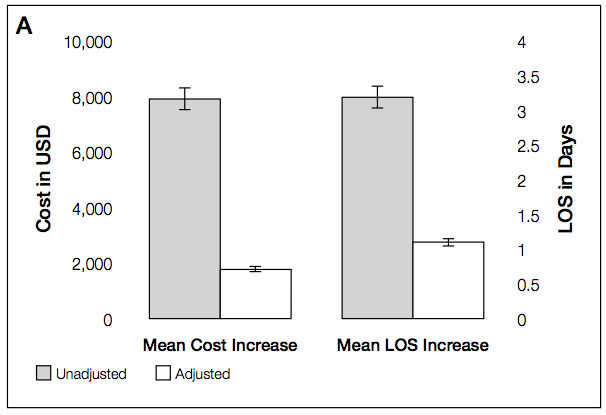
Getting AKI is expensive
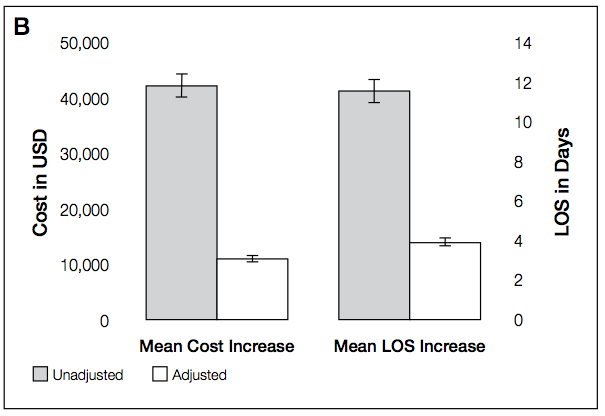
Getting AKI that requires dialysis is more expensive.
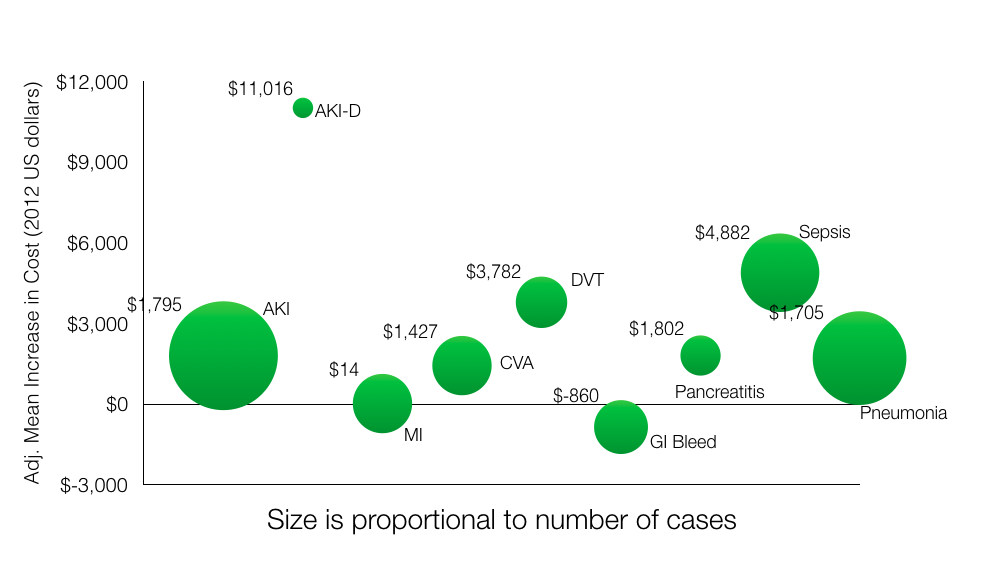
Compared to other diagnosis, AKI was the most common and AKI-D was the most expensive.
Someone explain to me how GI bleeds reduce the average cost of the hospitalization by 860 dollars? How does an MI increase the cost of care by only $14? This table was produced from the data in Table 2.
Discussion
It is amazing that AKI was the most common complication they examined despite using criteria which they know to have limited sensitivity, so the actual number of cases would be even larger. However the cases they missed are less severe (increases in creatinine of 0.3 mg/dL compared to 1.2 mg/dL) so presumably the costs would cost would come down. AKI-D does not suffer from this weakness, so it's extraordinary cost is not inflated by an artifact of the diagnosis of AKI-D
The authors justify the use of the adjusted costs:
Unlike previous studies, these analyses are fully adjusted for procedures and multiple hospital-level variables (such as teaching status, region, and bed number). These adjust- ments are important because procedures account for much of the incremental cost and LOS associated with AKI, and each hospital-level variable may increase the cost and LOS of an AKI hospitalization by 10% to 25%
At a yearly cost of $5.4 billion, the only condition that was more expesive than AKI (cost x prevalence) was sepsis at $7.7 billion. Hopefully this cost data will be used to justify additional research in treating and preventing AKI.