The agony and ecstasy of Bayesian Statistics.
Law 1: A strong intuition is more powerful than a weak test
law 3: Mostly Wrong
Law 3: For every perfect medical experiment, there is a perfect human bias.
The brevity ofThe Laws of Medicine makes it more powerful. The book can be devoured in a single morning, but the reader will still be left profoundly impacted.
Dr. Siddhartha Mukherjee challenges the reader to go beyond contemplating the three laws that make up the book, but to conceive and open one's eyes to other Laws. Today, with an expanding data-driven world, we discount our humanity. From the author’s note:
“It’s easy to make perfect decisions with perfect information. Medicine asks you to make perfect decisions with imperfect information.”
This imperfect information is then processed through the imperfect spectacles of the human mind.
In 1954 Dr. Richard Asher wrote that we are men of action, but every action is, and ought to be, preceded by a certain amount of thought. We should carefully examine these thought processes as they can be faulty. Dr. He says that crooked or dishonest thinking can occur in medicine & classifies crooked thinking in medicine under therapeutics, statistics, causes, words, etc. He says that the concept that a statistical relationship between two things automatically implies a causal relationship between them is “perverse.” He points out, for example, that statistics would show the incidence of erythroblastosis foetalis is twenty times less common in children of opium smokers. However, this should not obviously lead to prescribing opium in the maternity ward. These types of causal relationships are among our human biases that have existed from well before Dr. Asher’s publication over sixty years ago, and are present in today’s medical practice as stated in Law 3.
Law 1: a strong intuition is much more powerful than a weak test, and Law 3 are closely related. Law 1 can be paraphrased as “every diagnostic challenge in medicine can be imagined as a probability game.” Probability is based on objective factors such as prior organ damage and testing, but also the physician’s history taking, instincts, and interpretation of the data. One of my favorite passages in the book is when Dr. Mukherjee quotes Dr. Bernie Fisher: “In God we trust. All others must bring data.” However, being human, our biases can change the lens through which all this data is examined. If the data collector is flawed, does that not mean his accruement, analysis, and interpretation of the information is flawed? How do we account for this? Dr. Mukherjee says that reading a study inherently introduces human perception, arbitration, and interpretation – and hence involves bias. Bias is not only limited to research and those reading and analyzing the study. What bias can the subjects of the study introduce? One should consider the possibility of the Hawthorne Effect- when a human knows they are being observed, behavior changes. How do we account for these biases?
What about making medical decisions? Often complex decisions are made using mental heuristics and shortcuts to reduce complexity. These shortcuts develop over time with experience and increased knowledge in the field. Biases however, particularly cognitive biases, can easily creep in. While in medical school, I would hear of a symptom, or learn of a treatment, and try to apply this to all similar clinical situations (anchoring bias). Even experienced physicians are susceptible to similar biases. How often do we ask what is the data for established treatments? Sodium polystyrene sulfonate (Kayexelate) was approved based on two studies that barely deserve the name studies (no controls, confounders such as low K diet, diuretics, and other drugs that lower potassium). In 2011, the FDA issued a warning that Kayexelate was associated with colonic necrosis. For over fifty years Kayexelate was used without much consideration until there were significant complications in patients. Did the fact that Kayexalate was approved and was an old drug allow this complication to be overlooked for so long?
This brings me to the practice of evidence based medicine (EBM) and guidelines. In 1996 Dr. Sackett defined EBM as “the conscientious, explicit, and judicious use of current best evidence in making decisions involving the care of an individual patient. It integrates individual clinical expertise with the best available clinical evidence from systematic research.” How does this evidence come about? One thinks of a clinical question and the important outcomes to measure. The results are analyzed, and if found to be “good,” used in evidence based care. This evidence is often used to deliver a doctor-defined patient agenda. A medical encounter takes place and the health care provider focuses on what choices need to be made and carried out for the patient.
Has the research and medical decisions incorporated the patient? Did the research take into account the experience of their subjects? These questions are at the core of the movement to expand Patient Reported Outcome Measures (PROMs) and Patient Reported Experience Measures (PREMs) in our research agendas. We also must remember that EBM looks at the care of populations as opposed to individual patients. Dr. Shyaan Goh, an Orthopedic Surgeon from Australia, wrote to the British Medical Journal that the clinicians are the problem when EBM adversely affects clinical judgment. The clinician might not account for the quality or applicability of the evidence; they might not understand the rationale behind a guideline and not properly observe the guideline.
The question asked throughout this commentary is how do we account for these biases? How do we guard ourselves from allowing our own human instincts that may lead us astray? I think it is imperative to focus on the central figure of the story, the patient, not the health care provider. We have to take into account the individual who is experiencing the illness- what are their goals and expectations? A patient is not just a series of questions and tests.
As for the clinicians themselves, what other advice might be helpful? Well, Dr. Asher implored us to keep on the path of straight-thinking, regardless of the destination, to avoid crooked thinking. He quoted Rudyard Kipling’s Elephant’s Child to provide us with “helpers” to achieve this end:
“I keep six honest serving-men,
Their names are What and Why and When
and How and Where and Who.”
Maybe we should consider having these six helpers at our side aiding us to “hunt” and bring our biases to the forefront. Then, as Dr. Mukherjee says, we can confront bias head-on and incorporate it into the very definition of medicine.
Commentary by Beje Thomas, Nephrologist
NSMC intern, class of 2018
Additional Reading:
- Asher R. Straight and crooked thinking in medicine. BMJ 1954;2:460.
- Lehman Richard. Siddhartha Mukherjee’s three laws of medicine. BMJ 2015; 351 :h6708
- Accad, M. and D. Francis. "Does Evidence Based Medicine Adversely Affect Clinical Judgment?" BMJ (Clinical Research Ed.) 362,
- Greenhalgh T et al. Six ‘biases’ against patients and careers in evidence-based medicine. BMC Med 2015;13:200
- Goh S. The Problem with Evidence Based Medicine is really the Clinicians. (Letter to the editor). BMJ. 2018 July 18
- Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn’t. BMJ. 1996;312:71–72. doi: 10.1136/bmj.312.7023.71.
Law 3: For every perfect medical experiment, there is a perfect human bias.
It is indeed nice to have three laws - recall Newton, and perhaps more famously, Asimov’s three laws of Robotics. It's pithy, epigrammatic and attempts to ground us. The laws teach us humility even as research and innovation reach ever upwards. So what does Mukherjee mean by this third law?
He starts off with his fellowship in Oncology. The Human Genome Project had its great moment, and though the term ‘precision medicine’ had not even made it past a synapse, the oncology world was dealing with precisely engineered, monoclonal antibodies with fabulously unheard of outcomes. Following on the success of the VEGF inhibitor Imatinib (Gleevec), there was another ‘cousin’ that Mukherjee and his cohort of fellows were seeing used. The fellows saw dramatic positive results in their patients - but somehow, paradoxically, and in stark contrast, the actual clinical trial showed little benefit. How did this happen? Selection bias struck the fellows. They were handed patients from graduating fellows who had the most ‘educational value’ aka the patients doing well. On the other hand, the patients who did not do well were handed back to the attending physician. Like the parable of the broken window, one has to be careful about what is not seen. The patients who are lost to follow up may be lost because they are too sick to come back. Though this was not a perfect experiment that Mukherjee describes - it does illustrate a common enough bias - bring it up the next time an experienced colleague starts off with an ‘in my experience…’ to counter your meticulously gathered data. Vinay Prasad explains the responder bias, all too common in oncology, in a nice tweetorial here.
Another example cited by Mukherjee is the radical mastectomy - Halsted’s procedure, championed by a famous Hopkins surgeon in 1882. In a clever piece of naming, the radical makes one imagine that the roots of cancer have been eradicated, and it took nearly a century before the futility of the approach was revealed by randomized controlled trial. A clever study from Giovannucci showed an example of recall bias. In women with breast cancer, the diet history taken after the cancer diagnosis seemed to suggest that high fat intake was associated with cancer. However, a dietary history taken a decade prior to the diagnosis of cancer, from the same women, showed no similar association. The cancer diagnosis creates false memories. Food questionnaires, forgive the pun, should be taken with a pinch of salt.
But these are all epidemiological studies. Surely randomized controlled trials are not biased. The entire rationale is to prevent these kind of confounding, selection bias - or information biases to creep in. However, the trial methods do count. Though Mukherjee doesn’t go in to those aspects, blinding, allocation concealment, proper randomization are but some additional features of trial quality which can bias even the best laid plans. Check out the Cochrane risk of bias tool, which explains a few of these in detail. There is more to this of course. Should one change practice on the basis of a single small trial? Enter publication bais - or the shelf drawer (full of unpublished negative trials) bias. How about the more important issue of generalizability, or external validity? Does a psychology study of WEIRD individuals apply to all humanity? Surely not. Men and women are biologically different - but not for all conditions and surely not in response to all therapies. The need to do trials in all subpopulations is sometimes carried too far, however, in denying effective therapies to dialysis patients. Just because a trial has been done in the general population doesn’t mean the therapy will not work in dialysis patients. Generalizability should not be an excuse to practice renalism.
So, Mukherjee wants us to be bias hunters, on the look out for biases in every study. Eternal vigilance is always necessary.
Summary by Swapnil Hiremath, Ottawa
Law 2. Outliers by Mukherjee, not Gladwell.
“Single patient anecdotes are often dismissed…But here, exactly such an anecdote had turned out to be a portal to a new scientific direction.”
In The Laws of Medicine by Dr. Siddhartha Mukherjee, he describes a researcher who noticed an outlier in a clinical trial of a new drug for bladder cancer who responded to the treatment when others had not. Through genetic studies, they were able to find specific mutations in the tumor that conferred a higher likelihood of response, thus opening new avenues for therapy. He argues that you should pay attention to those outliers as much (or more) as you do the rest of the population, because they probably have something very valuable to teach us. I couldn’t agree more.
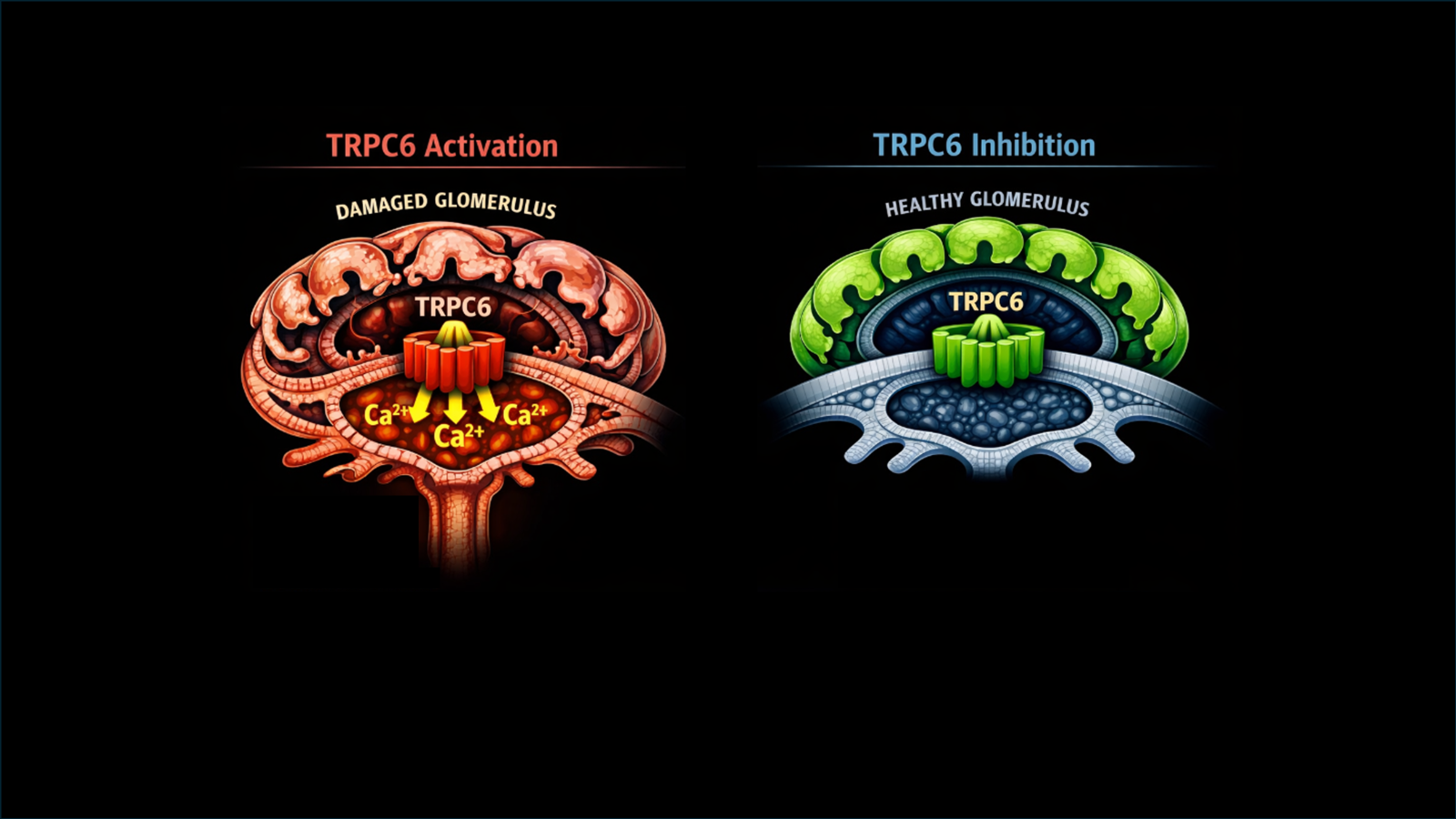
Pediatric nephrology is full of anecdotes that have informed nephrologists about the most basic kidney physiology. Congenital nephrotic syndrome was first described in the 1950s by Finnish nephrologists. While nephrologists were very familiar with typical minimal change nephrotic syndrome, these extremely rare children were different. They presented shortly after birth with massive proteinuria and died usually within the first year of life from infection. With improvements in supportive care, these children survived to kidney transplantation, however they still didn’t respond to our now standard treatment of steroids for nephrotic syndrome. It wasn’t until 1998, that the gene mutation responsible for this disorder was identified as nephrin (NPHS1), a slit diaphragm protein required for maintenance of the glomerular filtration barrier. This opened up a decade of fundamental research into the role of the podocyte in glomerular disease and helped to inform us about how the glomerular filtration barrier works.
In a less glomerulocentric view of the world (yes, I suppose there is such a thing), children with an unusual form of autosomal dominant hypertension were identified in the 1960s who had early onset disease with hypokalemia, suppressed renin and aldosterone, and responsiveness to triamterene but not spironolactone or dexamethasone. What on earth was going on in the tubule? It was long suspected that there was a defect in a sodium channel leading to salt and water retention, however the exact cause was elusive. Finally, in 1994, mutations in genes encoding the epithelial sodium channel (ENaC) [SCNN1B, SCNN1G] were found to be the cause of Liddle syndrome, opening new doors into research on blood pressure homeostasis and sodium handling in the kidney.
Genetic kidney diseases are one of my favorite parts about pediatric nephrology. You can learn so much about normal physiology when just one little thing goes wrong. But, you have to recognize the outlier and start to think about how they got there. Is this a thing of the past? Have all the genetic causes of disease been discovered already? Of course not. Keep your eyes open for that zebra.
Commentary by Michelle Rheault, Minneapolis
Law 2. Normals teach us rules; Outliers teach us laws
I search for patterns, always have. The logic of symptomatology is Glorious. I suspect this character trait is common in nephrologists. But revelling in the symptoms and signs that lead to a diagnosis and the investigative algorithm that refines the differential into the definite, has meant that I focus on what Siddhartha terms “inliers”. As I seek to make a patient “fit” my pre-conceived pathogenic model, I run the risk of missing a deeper truth. Brahe concentrated on the inliers and modelled the movement of the planets into concentric circles, frustrated that Mars wouldn’t fit this model. Kepler used the movement of the outlier, Mars, to reveal that all the planets orbit the sun in concentric ellipses. By concentrating on the range of normalcy we can only create rules, whereas “outliers” allow access to deeper laws.
Each outlier represents an opportunity to refine our understanding of illness. Asking why one patient in a thousand has responded to a drug, can reveal new disease pathways. David Solit used this approach to investigate why one woman’s advanced bladder cancer had a spectacular response to everolimus, while the drug appeared ineffective for the cohort as a whole. Sequencing that woman’s tumour showed multiple mutations, most interestingly in TSC1 and NF2, suggesting that these genes modulated the response to everolimus. The group went on to sequenced the same genes in the larger cohort and were able to segregate the group into responders and non-responders by the mutation in the TSC1 gene. In doing so they opened up new lines of enquiry and broadened the understanding of everolimus, bladder cancer, tuberous sclerosis and neurofibromatosis.
Through seeking to understand the outlier they opened up a deeper understanding of disease.
Now that case reports have fallen out of fashion, becoming almost impossible to publish and dismissed as anecdote, where are we to find our outliers? One option is to conduct “outlier rounds” as Siddhartha suggests, another is to seek out case report posters at conferences. But a further powerful option is to maintain an open dialogue with colleagues, whether in person or online, to tell our stories and to ask the deeper questions.
Cathy Quinlain
The Laws of Medicine: The Introduction
Before Siddhartha Mukherjee goes into the three laws of medicine he describes the origin of his search for the laws. It is a compelling read. Some of the truths he uncovers in these early pages are especially compelling. How about this gem from the Authors Note:
“It’s easy to make perfect decisions with perfect information. Medicine asks you to make perfect decisions with imperfect information.”
This is what makes doctoring so difficult. Even when the stakes are highest and lives are on the line we must make decisions with imperfect information. It is this stress that leads doctors to “overuse” radiology and laboratory services. We are always trying to perfect our information in the hope it will make our decisions “perfect.”
In describing how he started his search for the laws of medicine he tells the story of starting a medicine residency “in Boston.” He had a q3 call schedule. I had no idea those still existed in internal medicine in 1999. But I guess things move slowly in Boston. He does a wonderful job of describing the numbness that can come from a grueling residency,
”I ran through a park by night, and through friends by day”
His saving grace and only companion was a book by Lewis Thomas. Thomas was a medical resident in the 1930’s and described his experience of medicine in a slim paperback collection of essays titled, The Youngest Science.
Mukherjee describes medicine in the 30’s as emerging from a dark ages of quack cures that was followed by a period of therapeutic nihilism where the quackery was halted and physicians were limited to just documenting, classifying, and describing illness. In the 30’s physicians began to interpret the carefully collected observations and develop new therapies.
Mukherjee became drive to answer a seemingly simple question,
Is medicine a science?
Obviously, it was scientific in that it used techniques that were derived from phenomenally sophisticated science. But for medicine to be a science it had to have its own laws, independent from biology and pharmacology. If Medicine is a science it had to have laws, and so what are they? In his own words,
But does the “youngest science” have laws? It seems like an odd preoccupation now, but I spent much of my medical residency seeking the laws of medicine. The criteria were simple: a “law” had to distill some universal guiding principle of medicine into a statement of truth. The law could not be borrowed from biology or chemistry; it had to be specific to the practice of medicine...
...My search for the laws was not an attempt to codify or reduce the discipline into grand universals. Rather, I imagined them as guiding rules that a young doctor might teach himself as he navigates a profession that seems, at first glance, overwhelmingly unnavigable.
This introduction is beautifully written, full of fascinating stories and successfully reminds the reader how young the science of medicine is. We literally have patients in the hospital who are older than the science of medicine.
This introduction also brilliantly sets up the remainder of the book. I have played this introduction to the resident teams I lead and they both relate and are intrigued.
Summary written by Joel Topf, Detroit
#NephJCBookClub next Tuesday and Wednesday
The fourth annual NephJC Summer Book Club is here and we are reading and discussing, Siddhartha Mukherjee's The Laws of Medicine, Field Notes from an Uncertain Science.