Dr Hiremath gives the chronotherapy literature a Swap.
Revisiting the Ideal Time: The Case of Chronic Dialysis
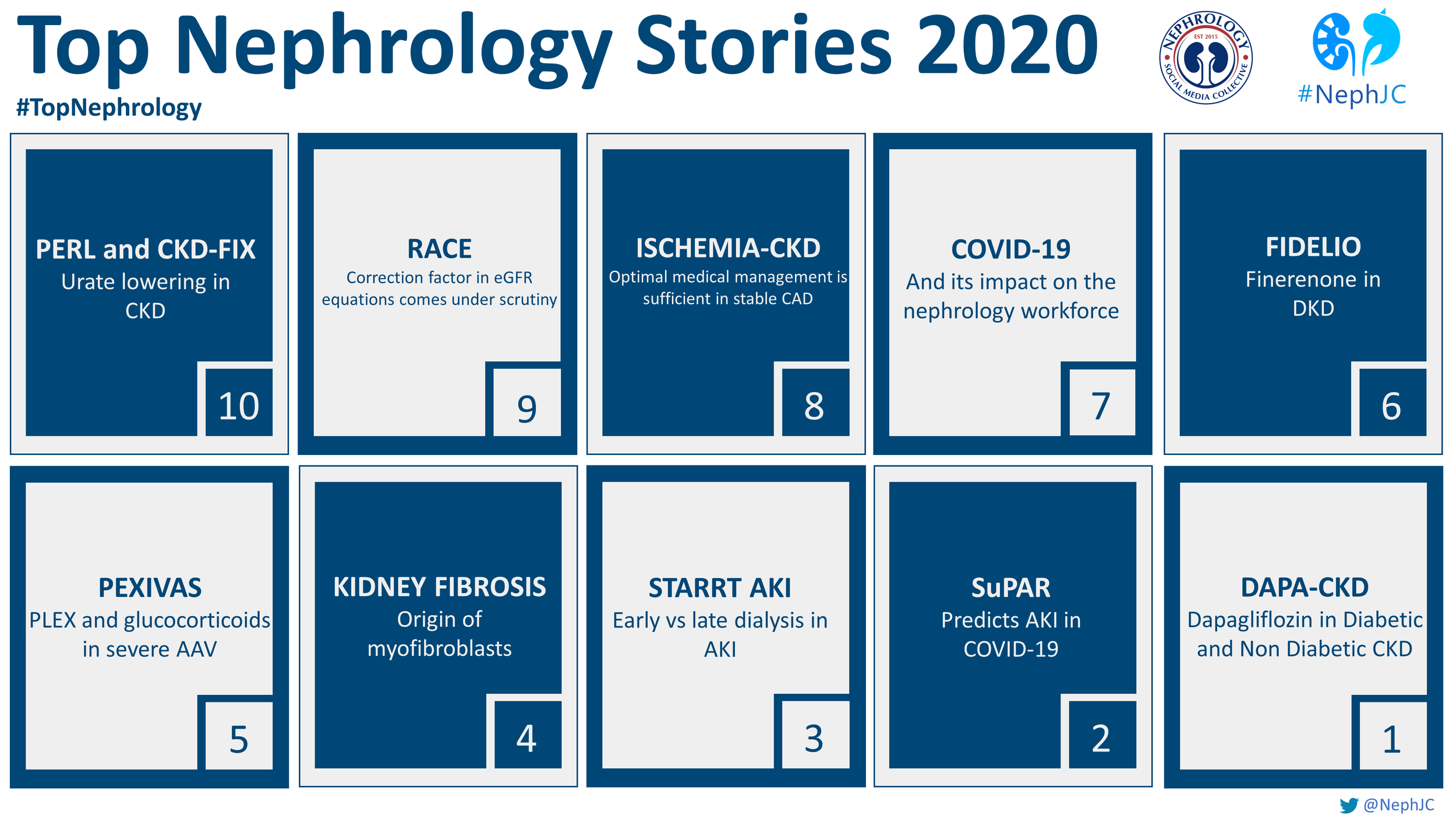
The Top Nephrology Stories of 2021
Time for some new Equations
Are Calcium-based Phosphate binders bad? A Rant/Commentary
VACCINES
Announcing #NephTrials
The Top Nephrology Stories of 2020
Renalism Returns with Remdesivir
ACUTE KIDNEY INJURY
As with all the other pages on COVID-19 here on NephJC, this page on AKI & the discussion are not meant to be treatment recommendations based on sound evidence. Our aim on this page is to merely discuss the science of what we know, and some of the biology and mechanisms as well as practical management aspects.
ACE2 and HYPERTENSION
There has been an unprecedented interest in this topic. Hence we have added more details and moved this section from the main page to a dedicated area with focus on hypertension and ACE2. Curated by Matt Sparks and Swapnil Hiremath, with additional expert input from the COVID-ACE2 workgroup
Newsflash: Numerous NSAIDs are Nephrotoxic
10 Steps to Read a Paper
Is Renal Denervation Innervated Again?
Kidney Transplant Disparities: UK data from the ATTOM study
Oral or IV Iron: Follow up from a previous #nephjc chat
A few months ago, we discussed this trial from Rajiv Agarwal and his team from Indiana, which found increased serious adverse vents with IV iron, in CKD patients. The latest issue of Kidney International now has some interesting correspondence, with two critical letters, and a substantive reply from Rajiv Agarwal.
Rajiv Agarwal
Among the criticism is one from Iain Macdougall and Simon Rogers, questioning the methodology - and why these results are different from the FIND-CKD trial (free PMC link), which did test a different IV iron formulation (iron carboxymaltose in FIND-CKD, iron sucrose in REVOKE), against a lower dose of oral iron. The reply from Dr Agarwal is worth reading in full, but this table highlights the details.
Table from Kidney International Vol 88, pg 1446-7