This week, we will discuss why a large registry cohort was needed to move past decades of scattered case reports and clarify the true risk of hydralazine‑associated vasculitis. When rare events hide in noise, only scale can reveal the signal. Can population‑level data finally bring this paradox into focus?
Can hydralazine trigger ANCA vasculitis?
A large registry cohort was essential to move beyond scattered case reports and finally quantify the true risk of hydralazine‑associated vasculitis. When rare events blur into background noise, only scale can clarify the signal. Can population‑level data sharpen the picture?
Check out Divya Bajpai VA
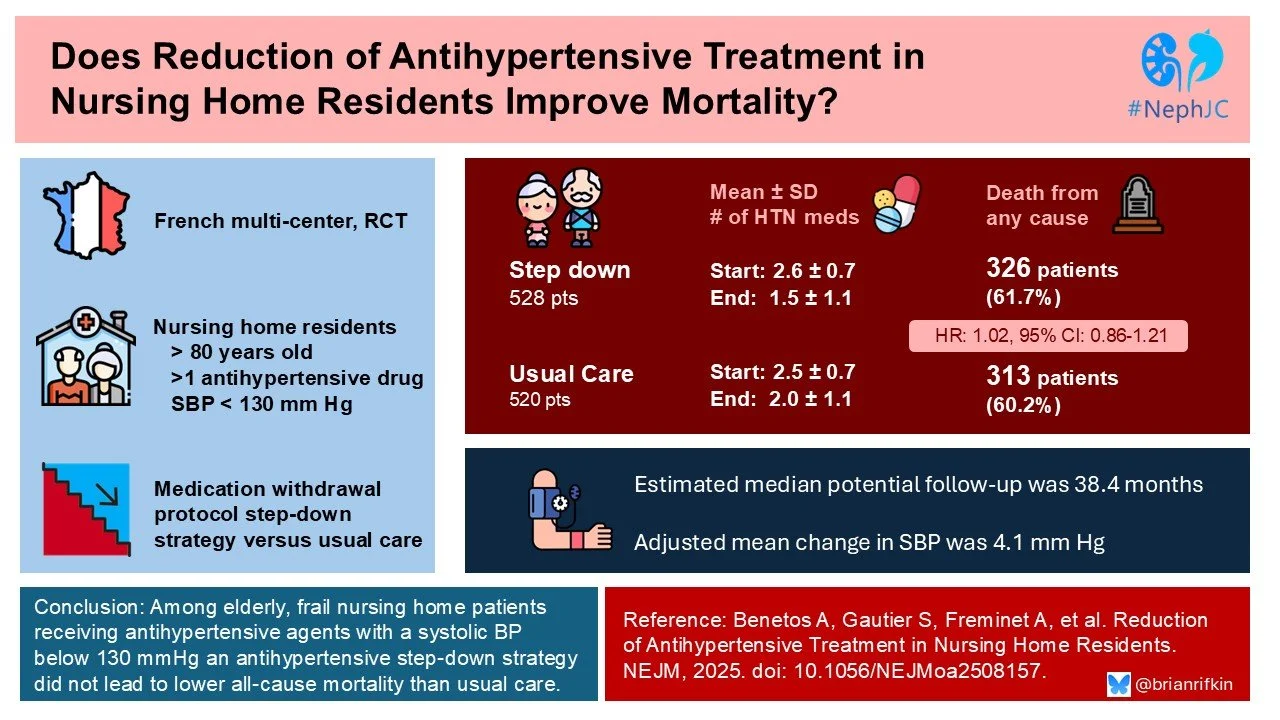
NephJC Shorts: Hypertension and The Extreme Elderly
ACC/AHA 2025 hypertension guidelines: what's new?
Check out the summary on AHA/ACC hypertension guidelines chat, done by NephJC intern Sridatta Pawar
ASIs Advance: NephJC Shorts on BaxHTN
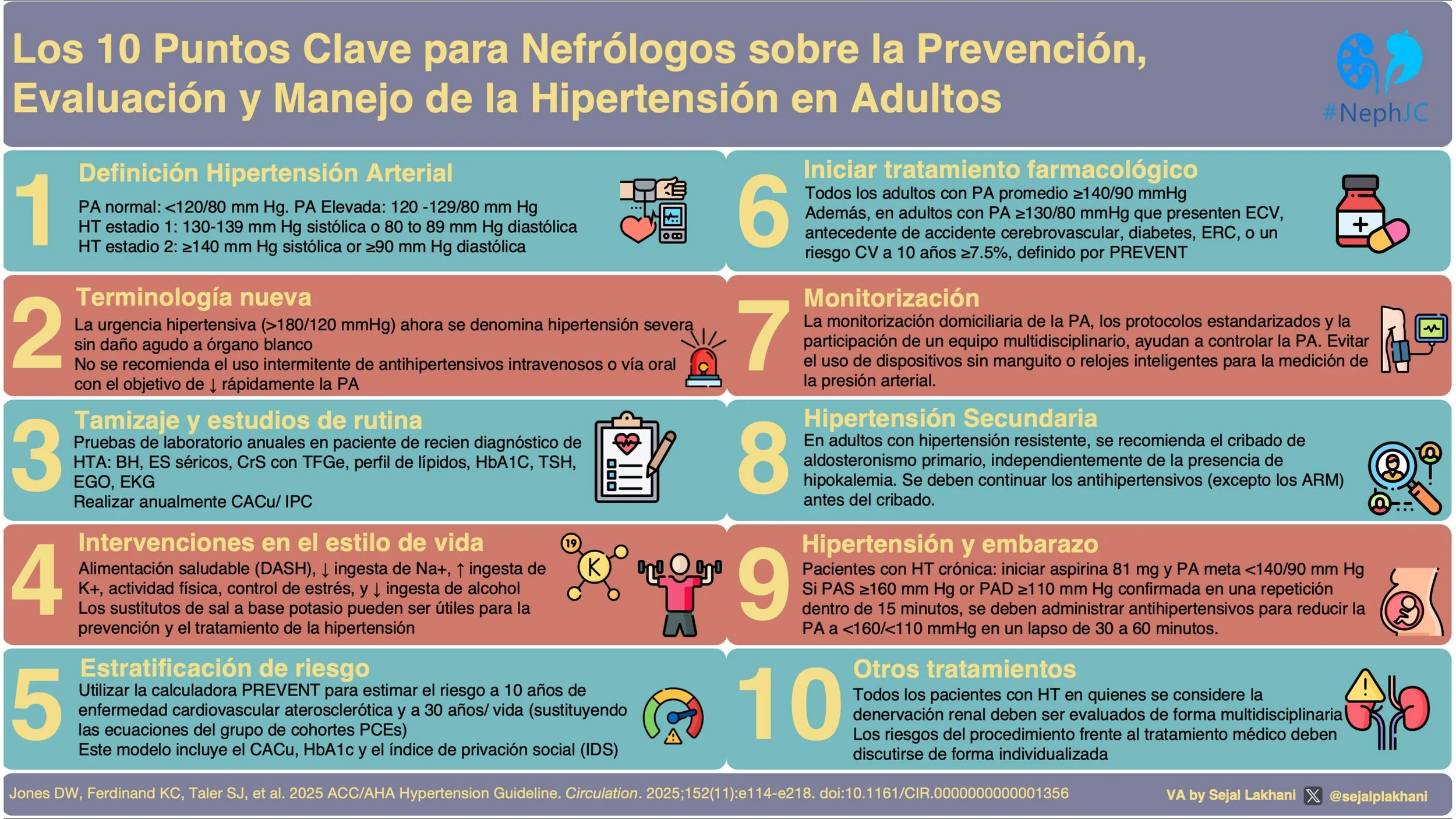
Guías AHA/ACC 2025 en Hipertensión: el resumen visual
La hipertensión arterial sigue siendo uno de los principales factores de riesgo modificables para enfermedad cardiovascular y enfermedad renal crónica. Las nuevas guías AHA/ACC 2025 han actualizado aspectos fundamentales sobre la prevención, la evaluación y el tratamiento de la hipertensión, con implicaciones directas para la práctica nefrológica.
Revisa el resumen visual creado por Dr Sejal Lakhani
visual abstract, Visual Abstract, sejal lakhani, Hypertension, HTN, ACC/AHA, 2025
The AHA/ACC 2025 Hypertension Guidelines visual abstract
New updated guidance on hypertension including screening for secondary causes, use of renal denervation, hypertension and pregnancy, risk assessment, monitoring and treatment.
Check out this wonderful VA by Dr Sejal Lakhani
PREVENT, Detect, Treat: What’s New in the 2025 Hypertension Toolkit
Advance-HTN: Return of the systolic order – Lorundrostat’s role in restoring balance
Does Lorundrostat Effectively Lower Blood Pressure in Uncontrolled Hypertension?
Stunning visual abstract summarizing NEJM study, by Priti Meena
Is a lower BP the road to better outcomes in diabetes?
How low is too low for blood pressure? Will BPROAD get to the bottom of this issue?
Underestimating primary aldosteronism?
Should we screen all individuals with hypertension for primary aldosteronism?
Hunting Primary Hyperaldosteronism: are MRAs a blindfold in adrenal vein sampling?
Undercover Aldosterone
BPROAD: Sprinting down the BP Road in Diabetes
The pressure is on! Unravelling the ESPRIT of Intensive vs Standard BP Control
This week, we will discuss the ongoing saga of blood pressure targets in patients with hypertension. This time its ESPRIT (Effects of Intensive Systolic Blood Pressure Lowering Treatment in Reducing Risk of Vascular Events) making a case for case for intensive BP control in most hypertensive individuals, including those with a history of diabetes and stroke.
NephJC Rewind: PATH-BP
We have been doing NephJC for over ten years and we feel, in that time we have covered the most important manuscripts in nephrology. With a decade of history NephJC has covered a large amount of the clinical evidence used in day to day clinical care. In fact I find myself sending links to old NephJC summaries pretty commonly and we would like to surface some of these older summaries from time to time. So here is out first NephJC Rewind
Last week JAMA Internal Medicine published this manuscript any Tim Anderson, Management of Elevated Blood Pressure in the Hospital—Rethinking Current Practice. Here, Dr. Anderson is trying to operationalize the work he has been doing for quite some time demonstrating the lack of efficacy and frank harm caused by treating inpatient hypertension. This has been explored in NephJC, Freely Filtered, and NephMadness. As part of this manuscript he supplied a flow chart that showed acetaminophen as a cause of hypertension:
I tweeted about this and a number of people asked about acetaminophen being listed as a cause of drug induced hypertension. This is where PATH-BP comes in (MacIntyre, Circulation 2022). This was a well done cross over trial with a two week washout. Patients took a gram of acetaminophen four times a day or a matched placebo.
The primary outcome was a change in mean daytime systolic ambulatory BP.
There was a statistically significant increase in mean daytime systolic ambulatory BP of 4.7 mm Hg (95% CI, 2.9-6.6; P<0.0001) with acetaminophen compared with placebo.
This was not a mechanistic study so we don’t no why but it is possible that acetaminophen blocks renal prostaglandin synthesis just like NSAIDs do.
Take a look at NephJC’s discussion as well as the original paper.